Cerebral Amyloid Angiopathy (CAA)
Summary
- Cerebral amyloid angiopathy is characterised by amyloid-β deposition in cerebral blood vessels
- Typically presents with lobar haemorrhages in older adults
- Imaging findings include microbleeds, cortical superficial siderosis, and white matter hyperintensities
Pathophysiology
- Accumulation of amyloid-β protein in walls of cortical and leptomeningeal vessels
- Leads to vessel wall weakening and increased risk of haemorrhage
- Associated with Alzheimer's disease but can occur independently
- Genetic factors (e.g., APOE ε4 allele) increase susceptibility
Demographics
- Primarily affects older adults (>55 years)
- Prevalence increases with age
- No significant gender predilection
- More common in individuals of European and Asian descent
Diagnosis
- Clinical presentation:
- Lobar intracerebral haemorrhage
- Transient focal neurological episodes
- Cognitive decline
- Boston criteria for CAA diagnosis:
- Definite: Full postmortem examination
- Probable: Clinical data and MRI findings
- Possible: Clinical data with limited MRI
Imaging
- CT findings:
- Lobar haemorrhages, often multiple and recurrent
- Subarachnoid haemorrhage
- MRI findings:
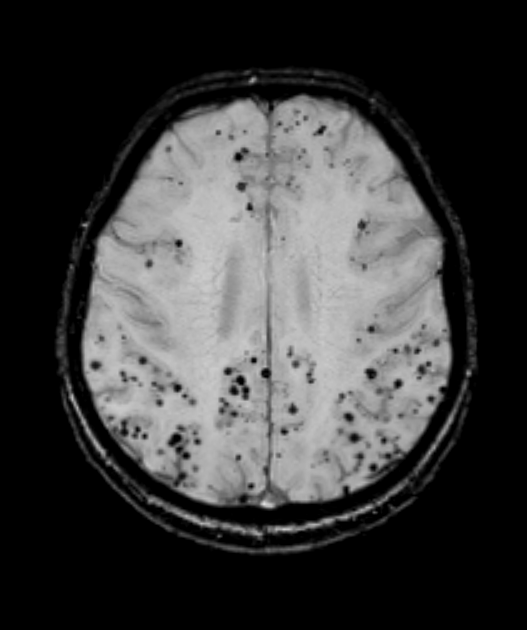
- Gradient-echo (GRE) or susceptibility-weighted imaging (SWI):
- Microbleeds in cortical/subcortical regions
- Cortical superficial siderosis
- T2-weighted and FLAIR:
- White matter hyperintensities
- Enlarged perivascular spaces in centrum semiovale
- PET imaging:
- Amyloid PET can detect vascular amyloid deposition
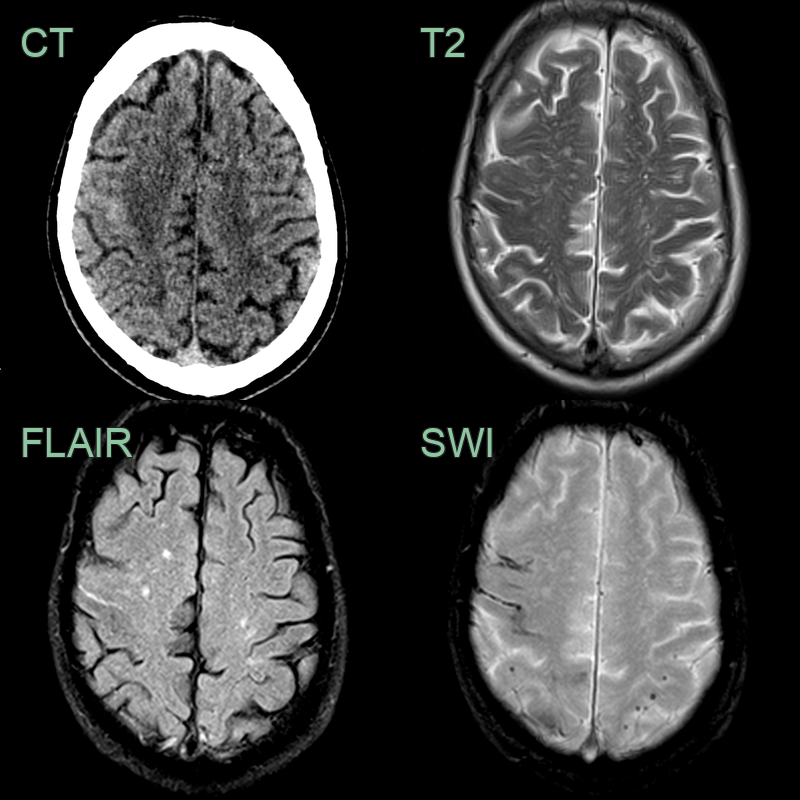
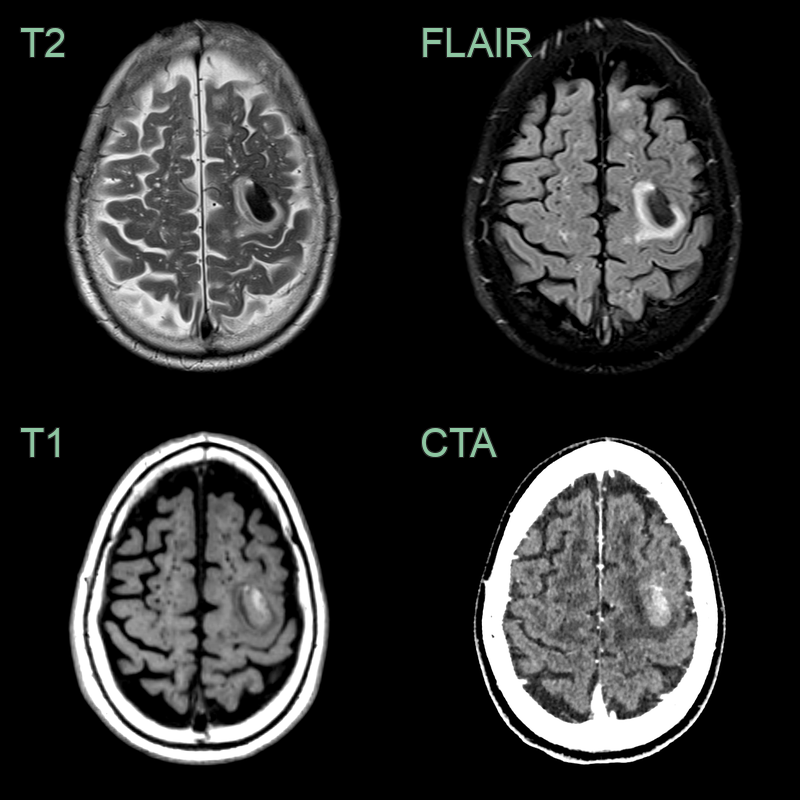
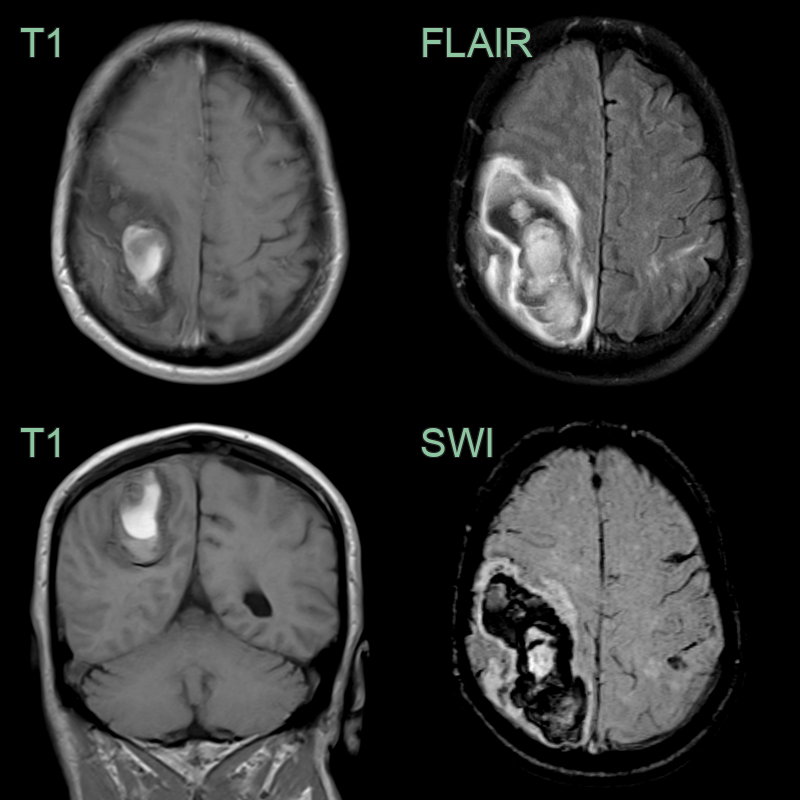
- 75-year-old patient presented with abnormal sensation in the left arm.
- CT showed blood product in the right pre-central gyrus.
- On MRI, there was sulcal hyperintensity on FLAIR consistent with recent blood product.
- Enlarged perivascular spaces, mutli-spot small vessel disease, superficial siderosis and lobar microhaemorrhages indicated a diagnosis of TFNEs secondary to CAA.
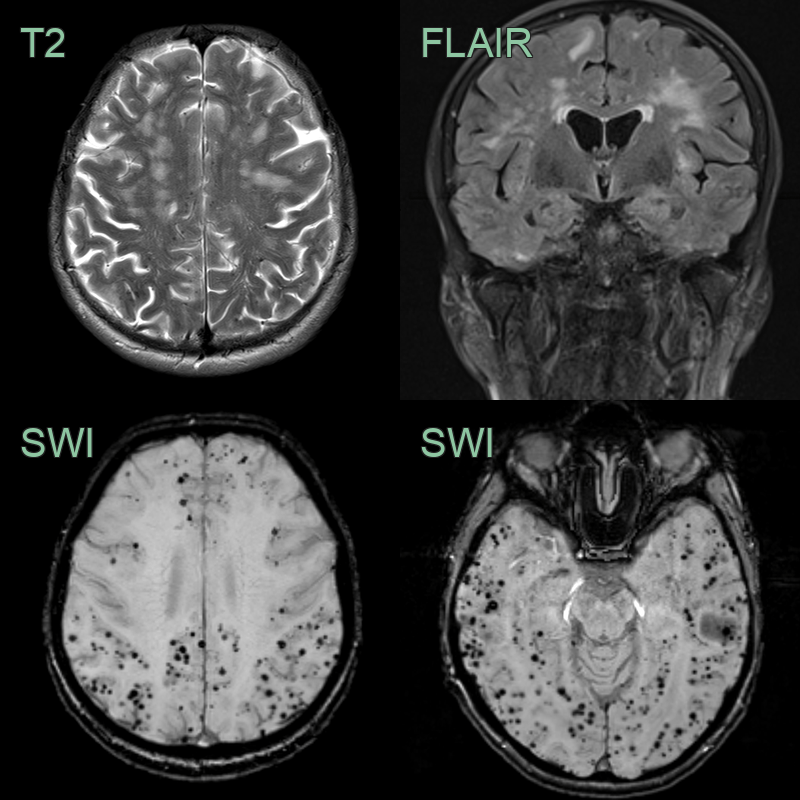
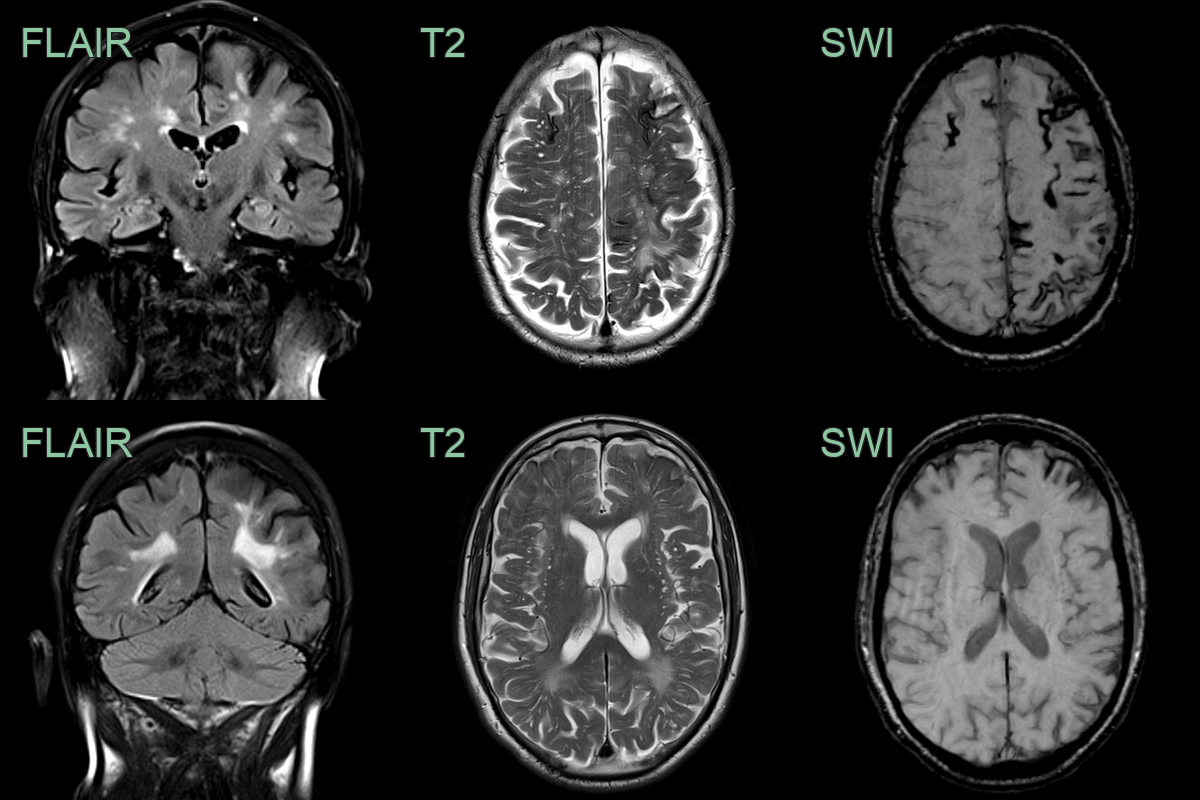
- Multi-spot small vessel disease, enlarged perivascular spaces, lobar microhaemorrhages, and extensive superficial siderosis indicate cerebral amyloid angiopathy.
- There was sulcal FLAIR hyperintensity in the right superior frontal sulcus and the left calcarine sulcus (not shown) that were associated with the left sided motor and right visual field TFNEs.
- 75-year-old patient presented with affecting right arm weakness.
- The initial MRI showed a lobar haemorrhage affecting the left precentral gyrus. There was a multi-plot pattern of (posterior-predominant) small vessel disease, many enlarged subcortical perivasular spaces, and extensive superfial siderosis but only a few few lobar microhaemorrhages.
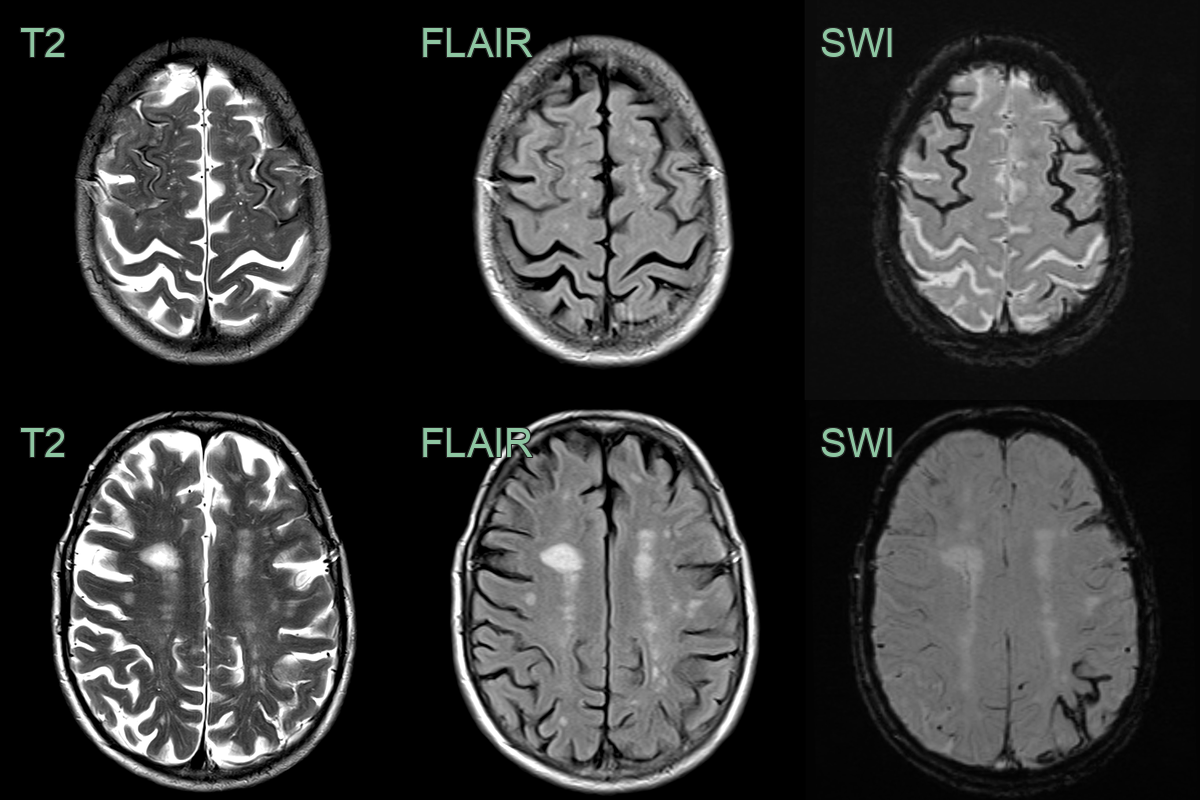
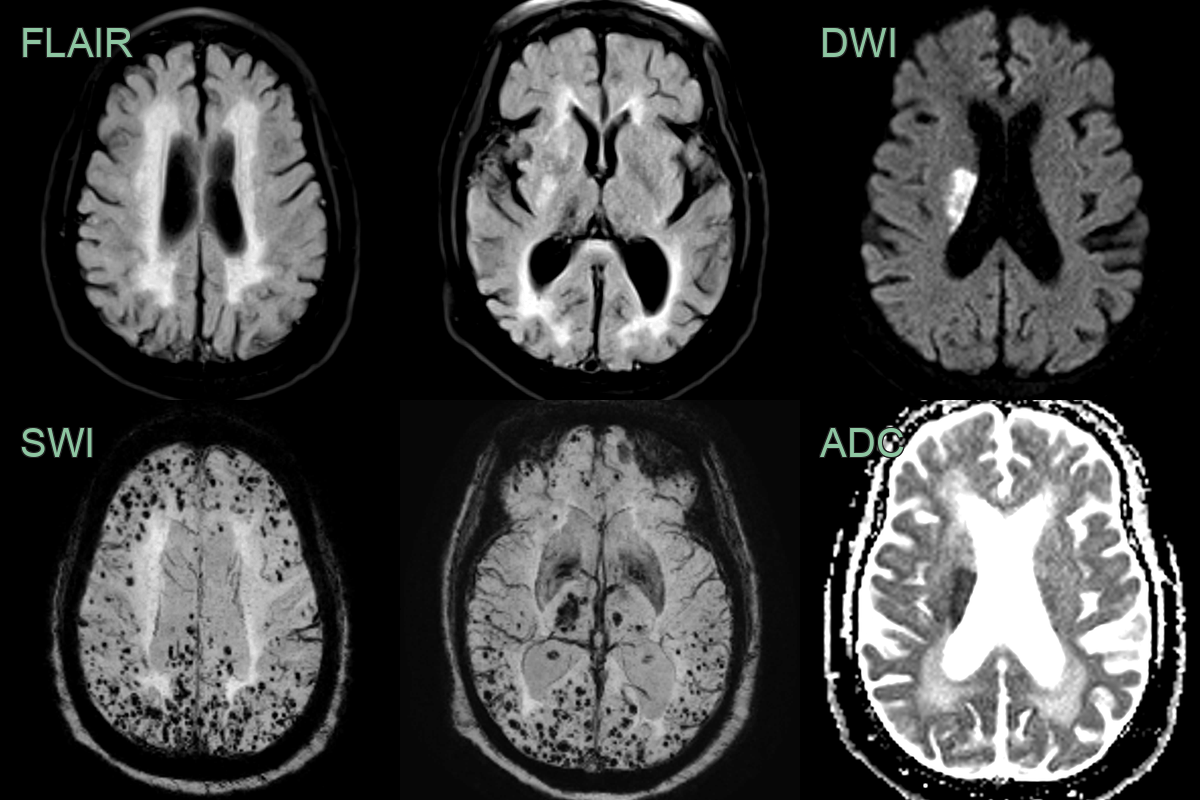
- A 75-year-old patient presented with left sided weakness.
- MRI showed an acute infarct in the right corona radiata.
- SWI showed florid microhaemorrhages in a mixed distribution - both deep (likely representing hypertensive arteriolosclerosis) and lobar (likely representing cerebral amyloid angiopathy).
- A 65-year-old patient presented with headache and left sided weakness.
- MRI showed a large lobar haematoma in the right parietal lobe.
- There was a trace of acute blood in the left post-central gyrus (based on FLAIR hyperintensity).
- While there were no white matter features of CAA, the combination of the superficial siderosis over the left frontal lobe and the lobar haematoma were sufficent to meet criteria for probable CAA.
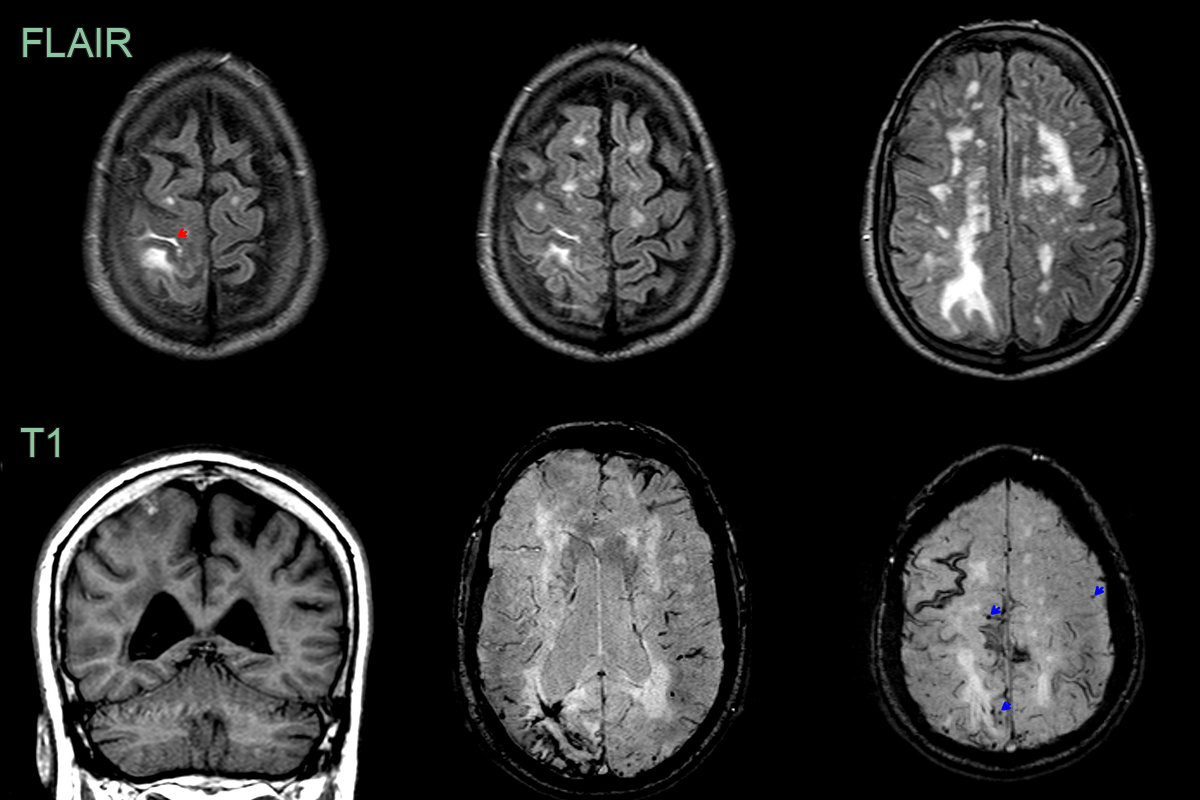
- A 70-year-old patient presented with transient senory distrubance in the left arm and left side of the face.
- MRI showed subarachnoid blood/effusion in the right central sulcus (red arrows) as a cause of the TFNE.
- SWI showed cortical microhaemorrhages (green arrows) and many areas of superficial siderosis.
Treatment
- No specific treatment for CAA itself
- Management focuses on:
- Blood pressure control
- Avoidance of anticoagulants and antiplatelet agents when possible
- Symptomatic treatment of seizures if present
- Acute haemorrhage management:
- Reversal of anticoagulation if applicable
- Neurosurgical intervention in select cases
- Potential future therapies:
- Anti-amyloid immunotherapies
- BACE1 inhibitors to reduce amyloid-β production
Differential diagnosis
| Differential Diagnosis | Distinguishing Feature |
|---|---|
| Hypertensive haemorrhage | Typically occurs in deep brain structures; CAA affects lobar regions |
| Ischaemic stroke | Absence of microbleeds on gradient-echo MRI sequences |
| Cerebral venous thrombosis | Presence of filling defects in venous sinuses on imaging |
| Cerebral vasculitis | Beaded appearance of vessels on angiography |
| Multiple sclerosis | Ovoid periventricular lesions on MRI |
| CADASIL | White matter lesions in anterior temporal lobes and external capsule |