Cerebral Malaria
Summary
- Severe complication of Plasmodium falciparum infection affecting the central nervous system
- Characterized by impaired consciousness, seizures, and coma
- Diagnosis based on clinical presentation, blood smears, and neuroimaging findings
Pathophysiology
- Caused by sequestration of parasitised erythrocytes in cerebral microvasculature
- Leads to:
- Microvascular obstruction
- Endothelial activation
- Blood-brain barrier disruption
- Cerebral edema
- Inflammatory response contributes to neurological damage
- Potential long-term cognitive and neurological sequelae
Demographics
- Most common in children under 5 years in sub-Saharan Africa
- Also affects adults in regions with lower malaria transmission
- Travellers from non-endemic areas at risk when visiting malaria-endemic regions
- Mortality rate ranges from 15-25% despite treatment
Diagnosis
- Clinical criteria:
- Unarousable coma (Glasgow Coma Scale ≤9)
- Exclusion of other causes of encephalopathy
- Laboratory findings:
- Positive blood smear for P. falciparum
- Rapid diagnostic tests for malaria antigens
- Lumbar puncture to rule out other causes of coma
- Neuroimaging to assess complications and exclude differential diagnoses
Imaging
- CT findings:
- Brain swelling (50-75% of cases)
- Focal hypodensities suggesting infarction
- Rarely, hemorrhage
- MRI findings:
- More sensitive than CT for detecting subtle abnormalities
- T2 and FLAIR hyperintensities in:
- Cortical grey matter
- Basal ganglia
- Corpus callosum
- Brainstem
- Diffusion-weighted imaging may show cytotoxic edema
- Susceptibility-weighted imaging can detect microhemorrhages
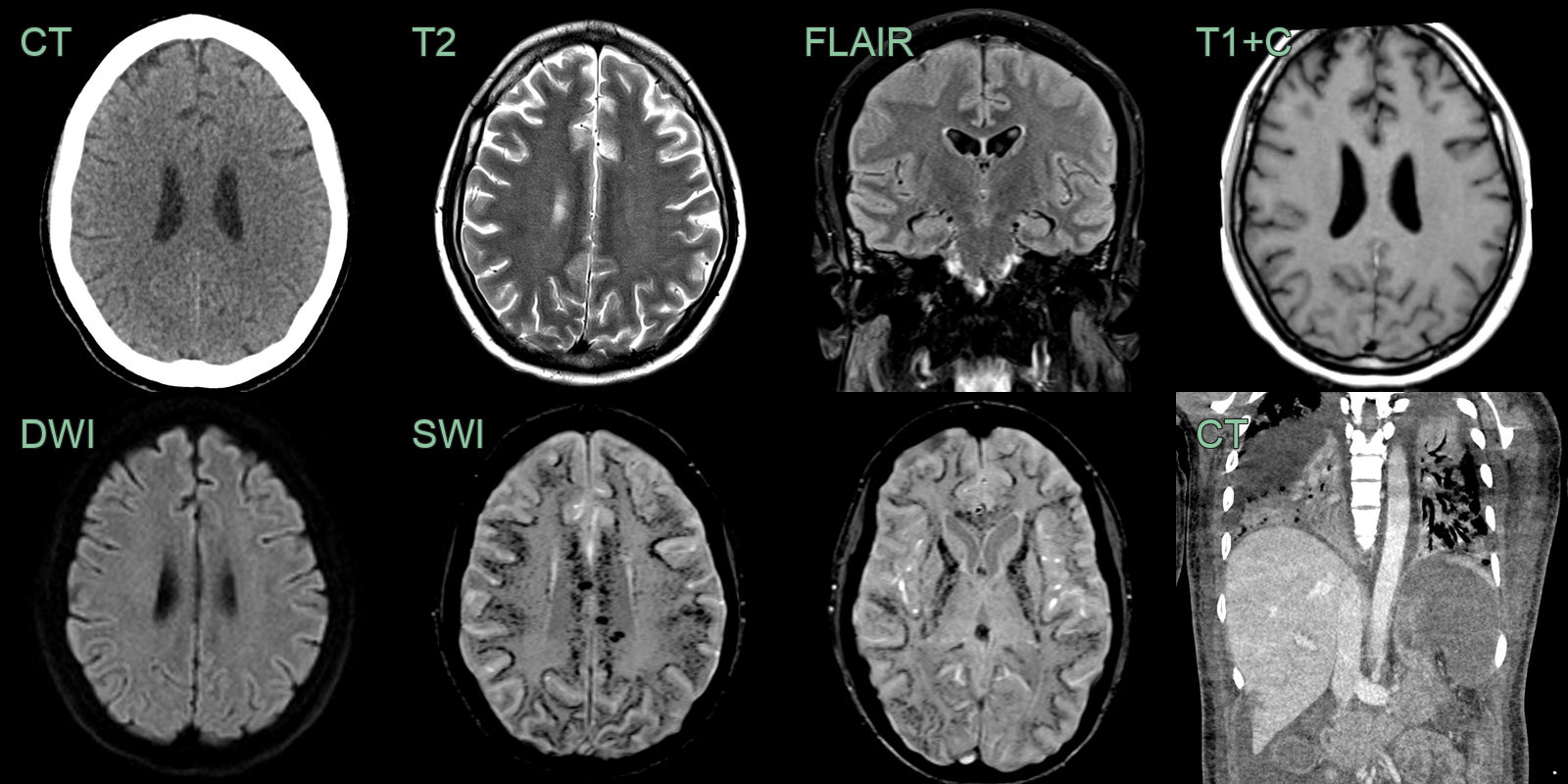
- A 40-year-old patient became obtunded 1 month after return from a region endemic for malaria.
- MRI showed the brain parenchyma appearing normal on T2 and FLAIR and DWI - there was no edema or ischemic changes.
- However, SWI showed extensive juxtacortical and deep white matter foci of susceptibility artefact (representing microhemorrhages and/or microthromb).
- Chest imaging showed bilateral lung consolidation, spenomegaly (with infarction) and small regions of hepatic infarcts.
Treatment
- Prompt administration of intravenous antimalarial drugs:
- Artesunate as first-line treatment
- Quinine as an alternative if artesunate unavailable
- Supportive care:
- Management of seizures
- Correction of hypoglycaemia and electrolyte imbalances
- Mechanical ventilation if required
- Monitoring for complications:
- Cerebral edema
- Acute kidney injury
- Severe anemia
- Rehabilitation for neurological sequelae
- Prevention strategies in endemic areas:
- Insecticide-treated bed nets
- Indoor residual spraying
- Chemoprophylaxis for high-risk groups
Differential diagnosis
| Differential Diagnosis | Distinguishing Feature |
|---|---|
| Bacterial Meningitis | Neck stiffness, cloudy CSF with high white cell count |
| Viral Encephalitis | Focal neurological signs, CSF PCR positive for viral pathogens |
| Severe Sepsis | Blood culture positive, no malarial parasites on blood smear |
| Diabetic Ketoacidosis | High blood glucose, ketones in urine, no malarial parasites |
| Heat Stroke | History of heat exposure, hyperthermia, no malarial parasites |
| Intracranial Hemorrhage | Focal neurological deficits, CT scan shows bleeding |
| Drug Intoxication | History of drug use, toxicology screen positive |
| Metabolic Encephalopathy | Abnormal electrolytes or liver function tests |
| Typhoid Fever | Relative bradycardia, rose spots, positive blood culture for Salmonella |
| Leptospirosis | Conjunctival suffusion, jaundice, positive serology |