Corticobasal Degeneration (CBD)
Summary
- Rare neurodegenerative disorder characterised by asymmetric cortical and basal ganglia dysfunction
- Presents with progressive asymmetric rigidity, apraxia, and cortical sensory loss
- Imaging shows asymmetric cortical atrophy, particularly in frontoparietal regions
Pathophysiology
- Accumulation of hyperphosphorylated tau protein in neurons and glial cells
- Affects cortical and subcortical regions, particularly motor cortex and basal ganglia
- Progressive neuronal loss and gliosis in affected areas
- Associated with mutations in the MAPT gene in some cases
Demographics
- Typically affects individuals aged 60-80 years
- Slight female predominance (1.5-2:1)
- Estimated prevalence of 4.9-7.3 per 100,000 individuals
Diagnosis
- Clinical diagnosis based on characteristic symptoms and signs:
- Asymmetric limb rigidity and akinesia
- Limb apraxia
- Cortical sensory loss
- Alien limb phenomenon
- Supportive features:
- Myoclonus
- Dystonia
- Cognitive impairment
- Definitive diagnosis requires neuropathological confirmation
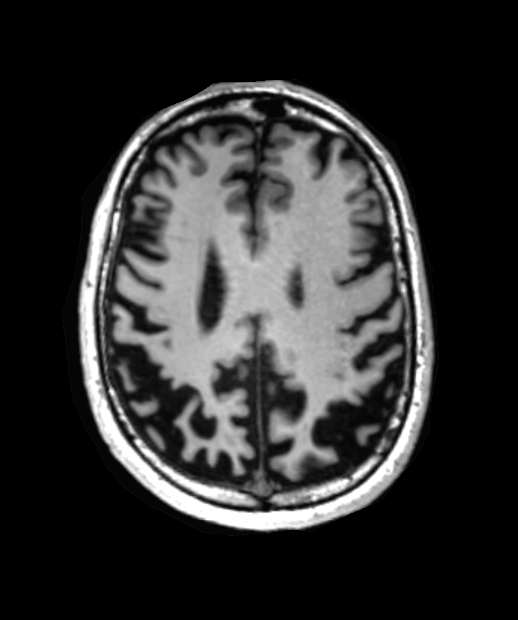
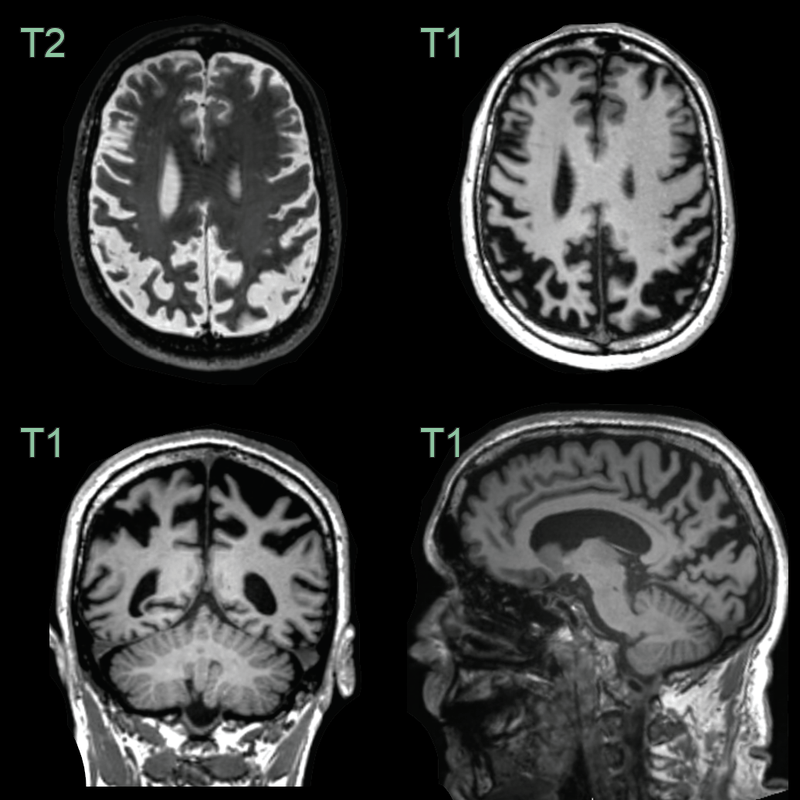
Imaging
- MRI:
- Asymmetric cortical atrophy, predominantly in frontoparietal regions
- Atrophy of basal ganglia, particularly putamen
- T2/FLAIR hyperintensity in subcortical white matter
- FDG-PET:
- Asymmetric hypometabolism in affected cortical regions and basal ganglia
- DaTscan (123I-FP-CIT SPECT):
- Asymmetric reduction in striatal dopamine transporter binding
Treatment
- No curative treatment available
- Symptomatic management:
- Levodopa for parkinsonian symptoms (often with limited response)
- Botulinum toxin injections for dystonia and muscle spasms
- Anticholinergics for drooling
- Physiotherapy and occupational therapy for mobility and daily living activities
- Supportive care:
- Speech and language therapy for communication difficulties
- Nutritional support
- Psychological support for patients and caregivers
- Ongoing research into tau-targeted therapies and neuroprotective agents
Differential diagnosis
| Differential Diagnosis | Distinguishing Feature |
|---|---|
| Progressive Supranuclear Palsy (PSP) | Prominent early vertical gaze palsy in PSP; less asymmetry compared to CBD |
| Parkinson's Disease | Better response to levodopa; tremor more common; less cortical involvement |
| Alzheimer's Disease | More prominent memory impairment; less motor symptoms |
| Frontotemporal Dementia | Less motor involvement; more behavioural and language symptoms |
| Multiple System Atrophy | More prominent autonomic dysfunction; cerebellar signs |