Grey Matter Heterotopia
Summary
- Neuronal migration disorder characterised by ectopic grey matter in abnormal locations
- Presents with seizures, developmental delay, and intellectual disability
- MRI shows nodular or band-like areas of grey matter signal intensity in abnormal locations
Pathophysiology
- Results from disrupted neuronal migration during fetal development
- Neurons fail to reach their intended destination in the cortex
- Genetic factors implicated, including mutations in DCX, FLNA, and ARX genes
Demographics
- Incidence: 0.05-0.1% in general population
- More common in females (X-linked forms)
- Can be diagnosed prenatally, in childhood, or in adulthood
Diagnosis
- Clinical presentation:
- Seizures (most common)
- Developmental delay
- Intellectual disability
- Focal neurological deficits
- Genetic testing for associated mutations
- Neuroimaging (MRI) is the gold standard for diagnosis
Imaging
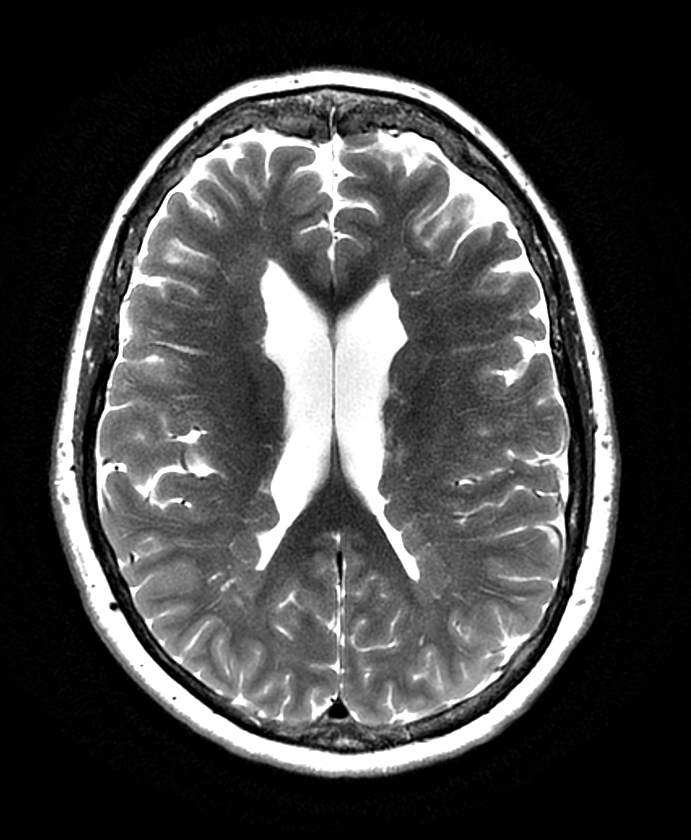
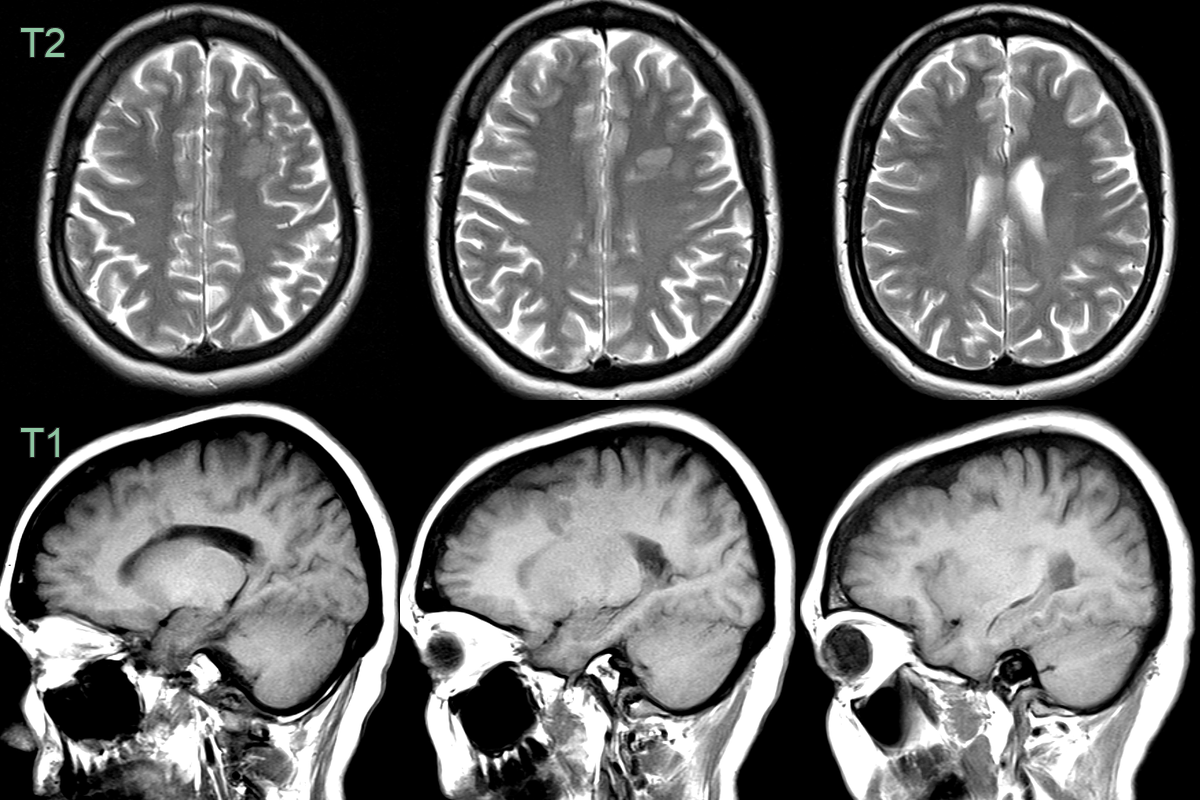
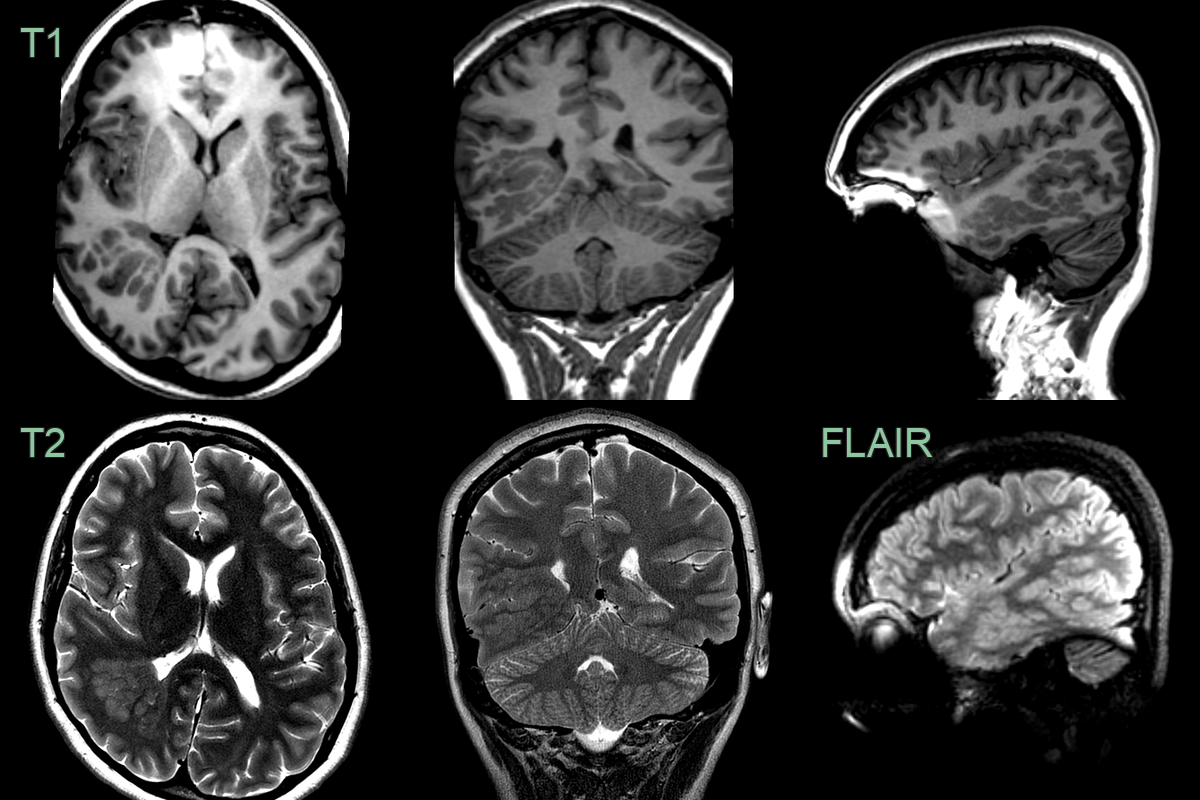
- MRI findings:
- T1-weighted: Isointense to normal grey matter
- T2-weighted: Isointense to normal grey matter
- FLAIR: Isointense to normal grey matter
- Types of heterotopia:
- Subependymal (periventricular nodular heterotopia)
- Subcortical
- Band heterotopia (double cortex syndrome)
- Associated findings:
- Corpus callosum abnormalities
- Cortical malformations (e.g., polymicrogyria)
- Cerebellar anomalies
Treatment
- Antiepileptic drugs for seizure control
- Surgical resection of heterotopic tissue in select cases
- Vagus nerve stimulation for refractory epilepsy
- Genetic counseling for familial cases
- Developmental and educational support for affected individuals
Differential diagnosis
| Differential Diagnosis | Differentiating Feature |
|---|---|
| Tuberous Sclerosis | Presence of cortical tubers and subependymal nodules |
| Focal Cortical Dysplasia | Abnormal cortical thickness and blurring of gray-white matter junction |
| Low-grade Glioma | Enhancement with contrast, mass effect, and surrounding oedema |
| Multiple Sclerosis | Ovoid periventricular lesions, "Dawson's fingers" |
| Subependymal Nodules | Typically calcified and located along ventricular walls |
| Periventricular Leukomalacia | Periventricular white matter injury, often with ventricular enlargement |
| Wallerian Degeneration | Linear white matter changes following specific tract distributions |
| Cerebral Infarction | Vascular territory distribution, evolution over time |
| Neurocysticercosis | Cystic lesions with eccentric scolex, often calcified |
| Cytomegalovirus Infection | Periventricular calcifications, ventriculomegaly |