Multisystem Atrophy - Parkinsonian Type (MSA-P)
Summary
- MSA-P is a neurodegenerative disorder characterised by parkinsonian features, autonomic dysfunction, and cerebellar ataxia
- Pathologically, it involves α-synuclein accumulation in oligodendrocytes and neuronal loss in multiple brain regions
- Imaging reveals characteristic patterns of atrophy and signal changes in the basal ganglia, cerebellum, and brainstem
Pathophysiology
- Accumulation of α-synuclein in glial cytoplasmic inclusions (GCIs) in oligodendrocytes
- Neuronal loss and gliosis in:
- Substantia nigra
- Striatum
- Globus pallidus
- Pontine nuclei
- Inferior olivary nuclei
- Cerebellar Purkinje cells
- Degeneration of autonomic nuclei in the brainstem and spinal cord
Demographics
- Typical onset: 50-60 years of age
- Slight male predominance (1.3:1)
- Estimated prevalence: 3-4 per 100,000 population
- More common in Caucasian populations
Diagnosis
- Clinical features:
- Parkinsonism (bradykinesia, rigidity, postural instability)
- Autonomic dysfunction (orthostatic hypotension, urinary incontinence, erectile dysfunction)
- Poor response to levodopa therapy
- Diagnostic criteria:
- Probable MSA-P: Parkinsonism + autonomic failure/urinary dysfunction
- Possible MSA-P: Parkinsonism + autonomic dysfunction or cerebellar syndrome
Imaging
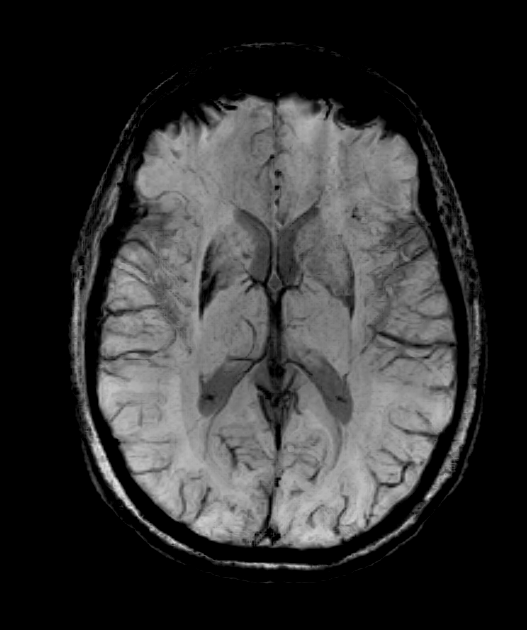
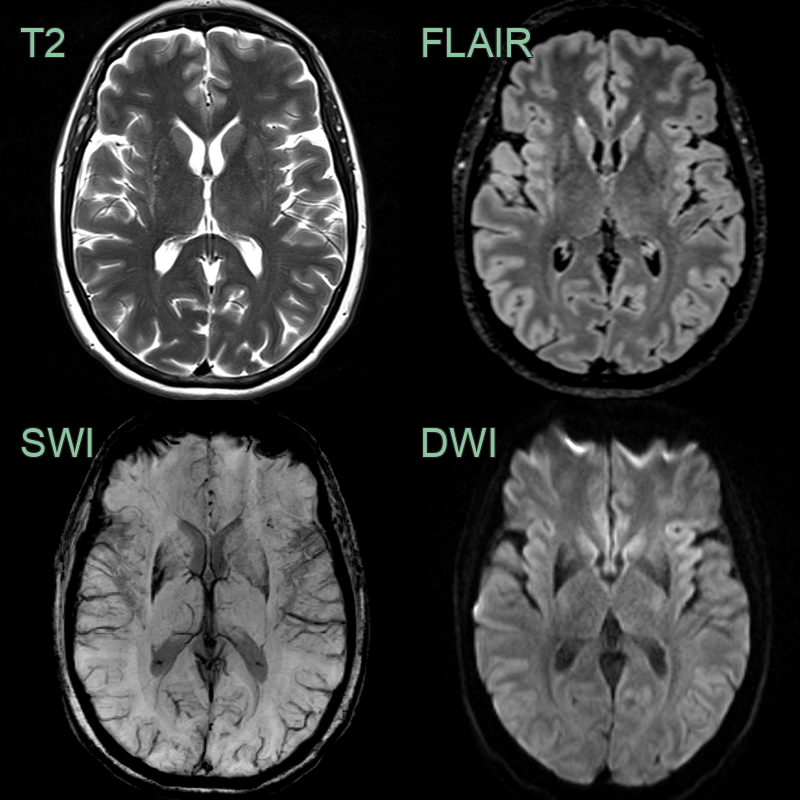
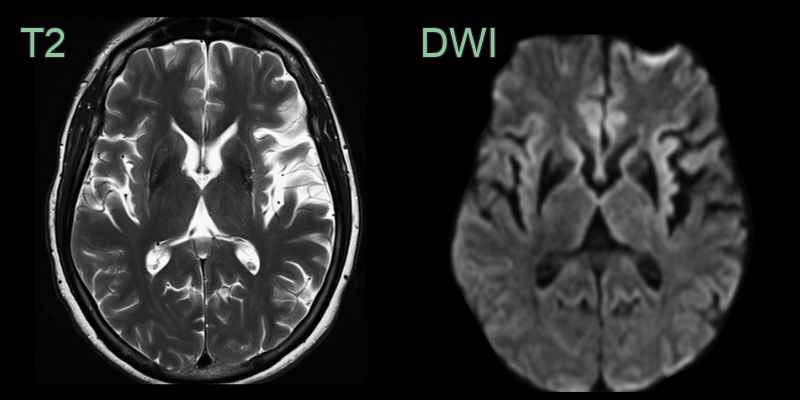
- MRI findings:
- Putaminal atrophy with T2 hypointensity
- "Hot cross bun" sign in pons (T2/FLAIR hyperintensity)
- Cerebellar atrophy
- "Putaminal rim" sign (T2 hyperintensity at lateral putaminal border)
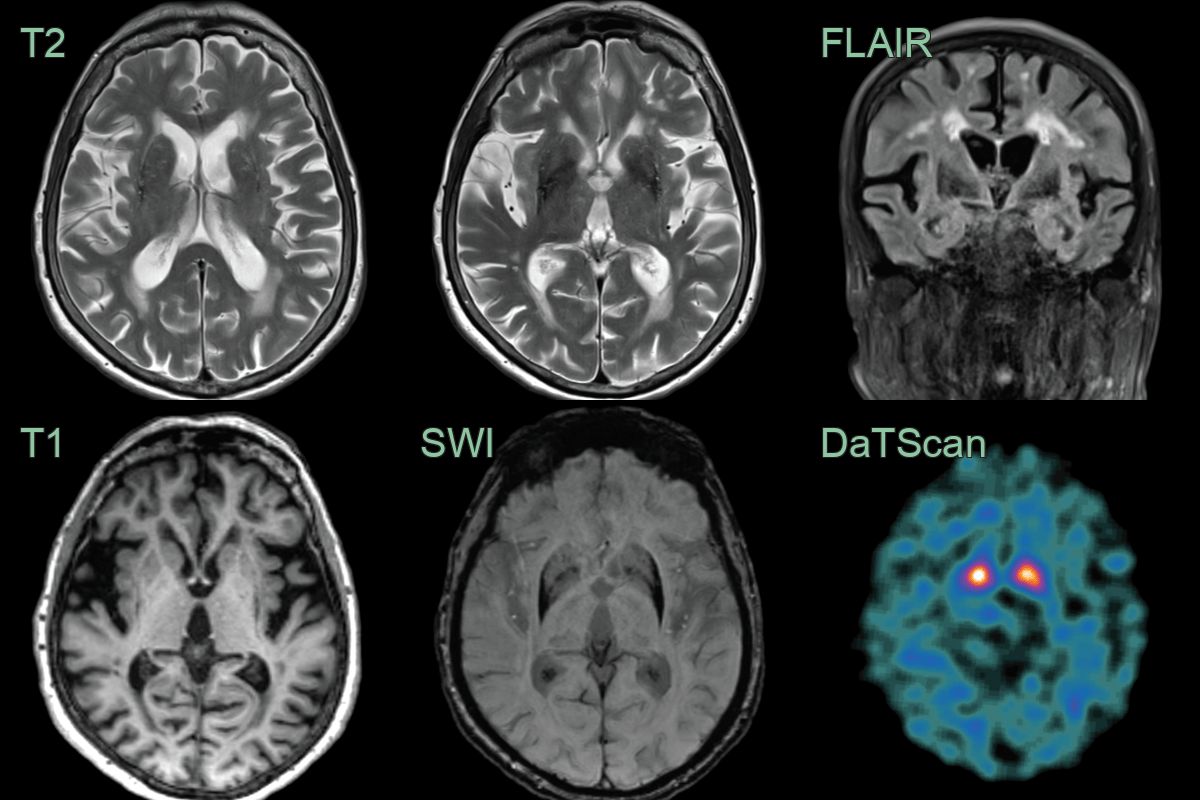
- DaTSCAN:
- Reduced striatal dopamine transporter uptake
- FDG-PET:
- Hypometabolism in striatum, brainstem, and cerebellum
- 80-year-old patient presented with asymmetric parkinsonism (left > right) with freezing and early falls with poor response to levodopa.
- MRI showed putaminal atrophy, susceptibility artefact and T2-hyperintensity along the lateral aspect of the putamina.
- DaTscan showed markedly reduced tracer uptake in the putamina bilaterally.
Treatment
- Symptomatic management:
- Levodopa for parkinsonism (often with limited response)
- Fludrocortisone or midodrine for orthostatic hypotension
- Anticholinergics for urinary symptoms
- Supportive care:
- Physical therapy
- Occupational therapy
- Speech therapy
- No disease-modifying treatments currently available
- Ongoing research into neuroprotective strategies and α-synuclein-targeted therapies
Differential diagnosis
| Differential Diagnosis | Distinguishing Feature |
|---|---|
| Parkinson's Disease | Poor response to levodopa; early autonomic dysfunction in MSA-P |
| Progressive Supranuclear Palsy | Vertical gaze palsy in PSP; more prominent cerebellar signs in MSA-P |
| Corticobasal Degeneration | Asymmetric limb apraxia and cortical sensory loss in CBD; more symmetric presentation in MSA-P |
| Dementia with Lewy Bodies | Early cognitive decline and visual hallucinations in DLB; more prominent autonomic dysfunction in MSA-P |
| Multiple System Atrophy - Cerebellar Type | Predominant cerebellar ataxia in MSA-C; more prominent parkinsonism in MSA-P |
| Vascular Parkinsonism | Stepwise progression and evidence of cerebrovascular disease on imaging in vascular parkinsonism |
| Drug-Induced Parkinsonism | History of causative medication use; typically resolves after drug discontinuation |
| Normal Pressure Hydrocephalus | Triad of gait disturbance, urinary incontinence, and cognitive decline; ventricular enlargement on imaging |