Parotid Abscess
Summary
- Parotid abscess is a localised collection of pus within the parotid gland
- Typically results from bacterial infection, often ascending from the oral cavity
- Presents with painful swelling of the parotid region, fever, and trismus
Pathophysiology
- Caused by bacterial infection, most commonly:
- Staphylococcus aureus
- Streptococcus species
- Anaerobic bacteria
- Infection usually ascends from the oral cavity via Stensen's duct
- Risk factors include:
- Dehydration
- Poor oral hygiene
- Immunosuppression
- Ductal obstruction (e.g., sialolithiasis)
- Progression of acute suppurative parotitis if left untreated
Demographics
- Can occur at any age, but more common in:
- Elderly patients
- Immunocompromised individuals
- Patients with poor oral hygiene
- No significant gender predilection
- Incidence has decreased with improved dental care and antibiotic use
Diagnosis
- Clinical presentation:
- Acute onset of painful swelling in the parotid region
- Fever and malaise
- Trismus (difficulty opening mouth)
- Purulent discharge from Stensen's duct
- Laboratory findings:
- Elevated white blood cell count
- Increased C-reactive protein and erythrocyte sedimentation rate
- Microbiological culture of pus or saliva to identify causative organism
Imaging
- Ultrasound:
- First-line imaging modality
- Hypoechoic or anechoic area within the parotid gland
- Internal echoes and septations may be present
- Increased vascularity in surrounding tissues
- CT with contrast:
- Low-density fluid collection with rim enhancement
- Surrounding inflammatory changes and oedema
- Useful for assessing extent and potential complications
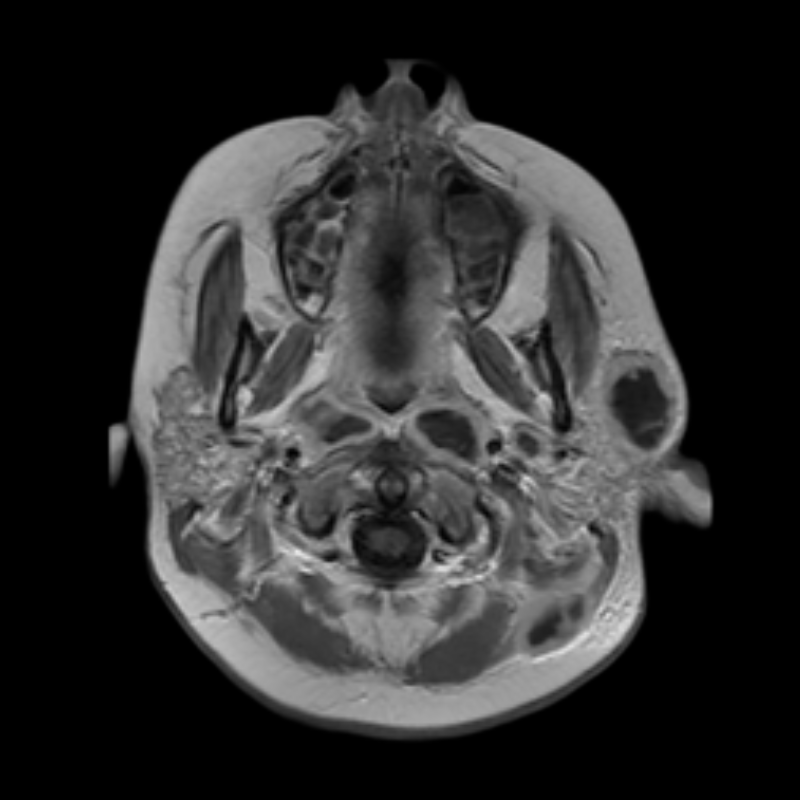
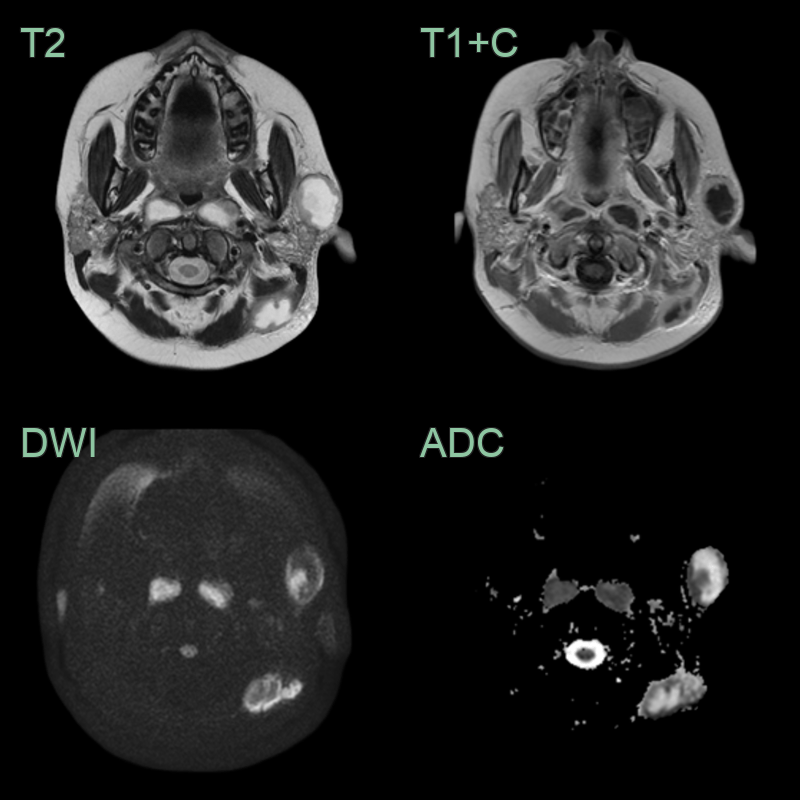
- MRI:
- Superior soft tissue contrast
- T1-weighted: hypointense lesion
- T2-weighted: hyperintense lesion with hypointense rim
- Diffusion-weighted imaging: restricted diffusion within abscess
Treatment
- Antibiotic therapy:
- Broad-spectrum antibiotics initially, then tailored based on culture results
- Common choices: amoxicillin-clavulanate, clindamycin, or cephalosporins
- Drainage:
- Ultrasound-guided aspiration for small, well-defined abscesses
- Surgical incision and drainage for larger or multiloculated abscesses
- Supportive measures:
- Adequate hydration
- Pain management
- Warm compresses to promote drainage
- Follow-up:
- Regular monitoring until complete resolution
- Address underlying risk factors to prevent recurrence
Differential diagnosis
| Differential Diagnosis | Differentiating Feature |
|---|---|
| Acute parotitis (without abscess) | Diffuse gland swelling without discrete fluid collection; no rim enhancement; no restricted diffusion |
| Parotid neoplasm | Solid mass without fluid signal; no rim enhancement; no inflammatory fat stranding |
| Intraparotid lymphadenitis | Discrete lymph nodes within parotid gland; no true glandular abscess cavity |
| Sialolithiasis | Calculus visible in Stensen's duct on CT; may cause duct dilatation without abscess formation |
| Branchial cleft cyst (second) | Well-circumscribed thin-walled cyst at angle of mandible or anterior to SCM; no restricted diffusion; no rim enhancement |
| Masseteric abscess | Collection centred in masseter muscle rather than parotid gland parenchyma |