Plasmacytoma
Summary
- Plasmacytoma is a localised neoplastic proliferation of plasma cells, occurring as solitary plasmacytoma of bone (SPB) or extramedullary plasmacytoma (EMP)
- Clinical presentation varies based on location, with bone pain common in SPB and mass effect in EMP
- Imaging plays a crucial role in diagnosis, staging, and treatment planning
Pathophysiology
- Monoclonal proliferation of plasma cells, producing a single immunoglobulin type
- Arises from post-germinal centre B cells
- May progress to multiple myeloma in some cases
- Genetic abnormalities include:
- Chromosomal translocations involving the immunoglobulin heavy chain locus
- Cyclin D dysregulation
- RAS mutations
Demographics
- Rare, accounting for <5% of plasma cell neoplasms
- Median age at diagnosis: 55-65 years
- Male predominance (male-to-female ratio 2:1 to 3:1)
- SPB more common than EMP (2:1 ratio)
- Higher incidence in African Americans compared to Caucasians
Diagnosis
- Clinical presentation:
- SPB: Bone pain, pathological fractures
- EMP: Mass effect, local symptoms based on location
- Laboratory findings:
- Serum and urine protein electrophoresis
- Serum free light chain assay
- Complete blood count, calcium, and creatinine levels
- Biopsy:
- Essential for definitive diagnosis
- Immunohistochemistry to confirm monoclonal plasma cell proliferation
- Exclusion of systemic involvement:
- Bone marrow biopsy (<10% clonal plasma cells)
- Skeletal survey or whole-body imaging
Imaging
- Radiography:
- SPB: Lytic lesion without sclerotic rim
- EMP: Soft tissue mass, may show bony erosion
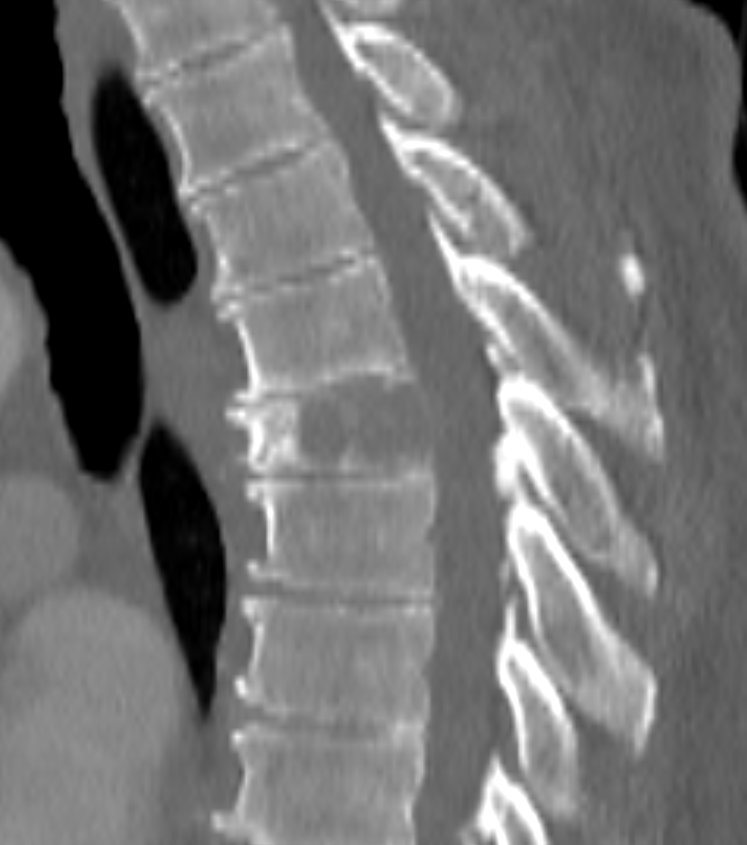
- CT:
- Higher sensitivity for detecting small lesions
- Useful for assessing cortical destruction and soft tissue extension
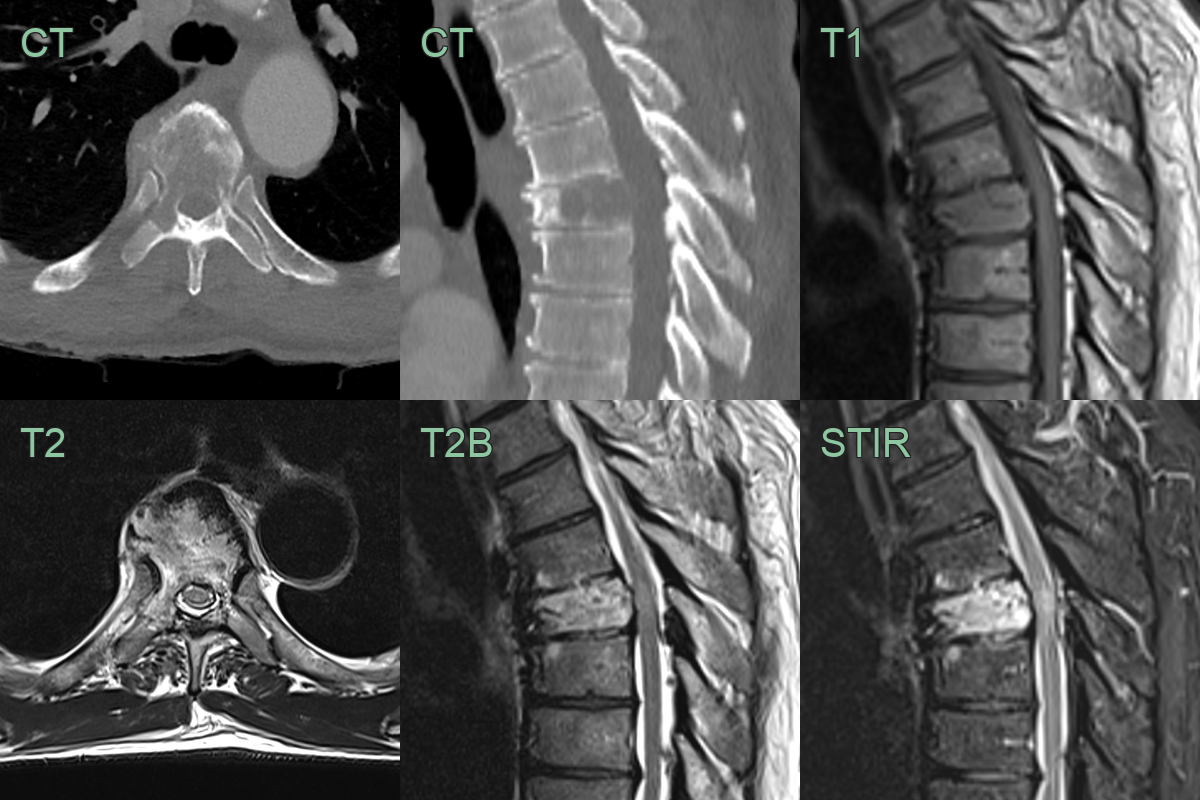
- MRI:
- Superior soft tissue contrast
- SPB: T1 hypointense, T2 hyperintense, enhancing lesion
- EMP: Well-defined, homogeneous mass with variable signal intensity
- PET/CT:
- High sensitivity for detecting lesions
- Useful for staging and treatment response assessment
- FDG-avid lesions
- Whole-body low-dose CT:
- Emerging modality for initial evaluation and follow-up
- Lower radiation dose compared to conventional skeletal survey
Treatment
- Radiation therapy:
- Primary treatment modality for both SPB and EMP
- Typical dose: 40-50 Gy in 20-25 fractions
- Surgery:
- Consider for unstable SPB or resectable EMP
- May be combined with radiation therapy
- Chemotherapy:
- Role in plasmacytoma management is controversial
- May be considered for large tumours or high-risk patients
- Follow-up:
- Regular monitoring for disease progression or transformation to multiple myeloma
- Includes serum protein electrophoresis, imaging studies, and bone marrow examination
- Prognosis:
- 5-year overall survival: 50-80%
- 10-year progression-free survival: 50-60%
Differential diagnosis
| Differential Diagnosis | Differentiating Feature |
|---|---|
| Multiple myeloma | Multiple punched-out lytic lesions; diffuse osteopenia; no isolated large solitary mass |
| Metastatic carcinoma | Multiple lesions; heterogeneous enhancement; associated soft tissue component; permeative bone destruction |
| Lymphoma | Permeative pattern with homogeneous enhancement; soft tissue mass; crosses disc space; no classic lytic punch-out |
| Giant cell tumour | Soap bubble appearance; epiphyseal location; adjacent to articular surface |
| Chordoma | Midline sacrum or clivus; T2 hyperintense with lobulated morphology; "honeycomb" trabeculation on CT |
| Osteosarcoma | Osteoid matrix on CT; aggressive periosteal reaction; cortical breakthrough; sunburst pattern |
| Ewing sarcoma | Onion-skin periosteal reaction; permeative pattern; aggressive soft tissue mass |
| Aneurysmal bone cyst | Fluid-fluid levels on MRI; expansile thin cortical shell; multiple internal septations |
| Fibrous dysplasia | Ground-glass appearance on X-ray, often polyostotic |
| Brown tumour | Associated with hyperparathyroidism, multiple lesions |